YOU ARE IN: > HOME > TEACHING & LEARNING > RESOURCES > TAKING AN OCCUPATIONAL HISTORY
Taking an Occupational History
(This is part of a larger resource intended to help undergraduates learn Occupational Medicine)
"It is at least as important to ask what man has the symptoms, as it is to ask what symptoms the man has."
A 30-year old man presented with episodic wheeze and cough. He gave as his occupation 'panel beater' - a trade involving the repair of the bodywork of crashed cars. Further questions were therefore directed at the possibility of exposure to sprayed paint and he said that this activity did take place in the garage, but by others and in a specially constructed booth; he was not exposed to the paint. By way of explanation, he was told that some two-part paints contain di-isocyanates and that these chemicals can cause occupational asthma. He then admitted that he had a second job in which he repaired car bodywork in his own garage at home. He had been using an isocyanate-based paint spray without any exhaust ventilation or respiratory protection! This proved to be the cause of his asthma, and after he had purchased appropriate respiratory protection and ventilation equipment he was able to continue this work without symptoms.
Introduction
An inadequate occupational history may result in labelling an illness as not "occupational" when it is, or vice-versa. It may result in missing the diagnosis altogether and in losing an opportunity (or even the last or only opportunity) of making the patient better and improving the fate of other workers. As in other aspects of medical history taking, two important lines of enquiry that must be followed are questions designed to elicit information about the:
- symptoms of existing underlying pathology
- background which may increase the likelihood of such pathology
In occupational medicine as in other aspects of medicine, the history taking may also fulfil other functions, for example in attempting to determine the response to a particular problem.
Remember that in occupational (and environmental) medicine it is just as important (perhaps more so) to ask what man has as symptoms as it is to ask what symptoms the man has.
Specific initial questions
In relation to the symptoms themselves, questioning may elicit:
- The organ system and type of pathological process involved e.g. wheeze, chest tightness and cough would suggest asthma, red itchy spots on a dry skin would suggest eczema/dermatitis.
But, most importantly in taking occupational history it is important to determine exposure:
A job title is not adequate
A full description of what the job entails is a bare minimum. What does an 'electro-plater' do, or a 'ram-block packer'!? The full job description may need to go back several years - mesothelioma for example can occur 40 years after first exposure to asbestos. Indeed in some circumstances it is important to take an occupational history going as far back as the patient’s first job (an environmental exposure history has rarely had to extend even to the pre-school years - as in the case of children who had played on tips containing asbestos or other hazardous substances).
The identity of any chemical exposures or other hazards must be clearly established

Colloquial terms may be used for chemicals e.g. "trike" (trichloroethylene), "perk" (perchloroethylene), or "monkey dung" (brown asbestos). Confirmation of the identity of a chemical might involve asking the patient to bring in a label or a hazard data sheet. For example if the history is suggestive of exposure to formaldehyde, then the label of the drum should confirm this.
It is important to try and determine the duration and intensity of exposure
Determining when exposure started, when it finished and how often it was repeated may be tedious but not very difficult. However determining the intensity of exposure by history taking is very difficult but the following are useful guides:
- How was the task done e.g. was an adhesive applied with a paint brush while the patient leant over it?
- Was the dust concentration so bad that one could not see clearly through it, or the noise so loud that communication was difficult?
- If control of exposure to a chemical appeared poor, what sort of quantities of it were handled?
- Was there any attempt at segregating harmful tasks, or providing local exhaust ventilation?
- Special questions are warranted in relation to personal protection. A response that the worker wears a mask is about as informative as a patient saying that he takes wee white pills. Many masks offer no protection whatsoever against gases vapours or dust e.g. surgical masks or old gauze masks, while "Nuisance Dust" masks of the sort often sold in DIY shops are not much better.
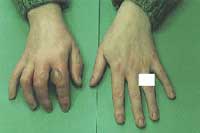 Different categories of harmful agents tend to have different and specific forms of personal protection. For example, masks designed for respirable dust will not protect from sulphur dioxide or solvent exposure. Thus gloves that may be suited to provide some protection against cement dust might not be of any use at all if exposed to petrol. The patient in the image (right) had high quality thick industrial black rubber gloves - but unfortunately they offered no protection from the alkylating agent which she was handling.
Different categories of harmful agents tend to have different and specific forms of personal protection. For example, masks designed for respirable dust will not protect from sulphur dioxide or solvent exposure. Thus gloves that may be suited to provide some protection against cement dust might not be of any use at all if exposed to petrol. The patient in the image (right) had high quality thick industrial black rubber gloves - but unfortunately they offered no protection from the alkylating agent which she was handling.
- The control measures e.g. local exhaust ventilation and personal protective equipment need to be regularly maintained. Ask the worker whether they are and who is responsible for this. in the example (below), a wide range of high quality, well maintained protective measures are in use.

Processing the historical information, and further questions.
There are a number of similarities between the processing of information in a clinical occupational medical history and the decisions regarding criteria for causal association that one encounters in epidemiology. Indeed many good occupational physicians practise both clinical medicine and epidemiology within the specialty of occupational medicine.
| Epidemiologic criteria for causality: |
Clinical Questions: |
| Temporality |
When in relation to exposure do / did the symptoms start? |
| Reversibility |
Do the symptoms improved when no longer exposed e.g. on holiday? |
| Exposure-response |
Are the symptoms especially worse when undertaking tasks or in areas with high exposures? |
| Strength of association |
Do other workers / patients suffer from similar symptoms associated with the same exposures? |
| Specificity |
What other exposures / causal factors could be responsible for the same symptoms? (Smoking perhaps?) |
|
Other data, or information processing: |
| Consistency |
Are there other reports of the same symptoms associated with or caused by the same exposure? |
| Analogy |
Even if there is no evidence to hand of identical exposures or circumstances resulting in the same symptoms, have similar agents/ chemicals of similar structure been implicated in the same symptoms of for example ... dermatitis, ... or asthma. |
| Biological plausibility |
Do the symptoms 'add up' in terms of what is known about the mechanisms of disease? |
Analogies between determining causality in an epidemiologic context (the Bradford-Hill criteria) in population studies, and when dealing with an individual patient in a clinical context.
Note: judgements in relation to the above should be made 'in the round'. For example: Just because a worker complaining of shortness of breath happens to be a smoker does not necessarily mean that his symptoms can be ascribed to smoking.
In conclusion, while taking an occupational history various avenues need to be explored:-
- One may wish to try and confirm suspicions by seeking links between various aspects of the history. For example if the patient has symptoms of asthma and is exposed to agents which might cause asthma, it will be reasonable to ask when the symptoms are at their worst and when they are at their best. Are they improved after a weekend off work, or better still after a fortnight’s holiday?
- Is there any other evidence of corroboration, such as similar symptoms in other workers?
- Alternative explanations might be explored. Is the patient a smoker? Does he engage in any "do it yourself" activities at home, hobbies or moonlighting? Find out more.
- While a working diagnosis is forming in your mind, you might also be considering ways to help and start asking relevant probing questions : What is the patient’s attitude?, the employer’s attitude? What resources and expertise may be available to provide further information or to assist rehabilitation?
Find out more about:
Acknowledgement
Part of this page has been adapted, with permission, from Practical Occupational Medicine (Copyright) - Arnold publishers.
 Different categories of harmful agents tend to have different and specific forms of personal protection. For example, masks designed for respirable dust will not protect from sulphur dioxide or solvent exposure. Thus gloves that may be suited to provide some protection against cement dust might not be of any use at all if exposed to petrol. The patient in the image (right) had high quality thick industrial black rubber gloves - but unfortunately they offered no protection from the alkylating agent which she was handling.
Different categories of harmful agents tend to have different and specific forms of personal protection. For example, masks designed for respirable dust will not protect from sulphur dioxide or solvent exposure. Thus gloves that may be suited to provide some protection against cement dust might not be of any use at all if exposed to petrol. The patient in the image (right) had high quality thick industrial black rubber gloves - but unfortunately they offered no protection from the alkylating agent which she was handling.
